Seen this question before? Click to switch to a different question.
Case presentation
An 84-year-old woman presents to the Medical Assessment Unit complaining of falls precipitated by standing-up, and dizziness when standing for long periods. PMH. Hypertension, depression, “ankle swelling”, urinary incontinence. DH. She normally takes bisoprolol 5mg oral daily, furosemide 40mg oral 12-hrly, amlodipine 5mg Oral daily, salbutamol inhaler 100 micrograms/ actuation two puffs 12-hrly, and fluoxetine 40mg oral daily. SH. Lives alone in sheltered accommodation. Her husband died about one year ago.
On examination
She appears cheerful and chatty. There is no peripheral oedema. BP is 130/85 mmHg lying and 108/70 mmHg standing, HR is 44/min.
Investigations
U 15.0 mmol/L (2.5 – 6.6), Cr 100 µmol/L (45 – 84), Na+ 131 mmol/L (133 – 145), K+ 4.4 mmol/L (3.5 – 5.5).
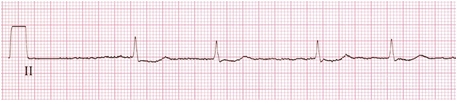
ECG